Empower staff to keep proven interventions top of mind
Wound care nurses know it can be a challenge to keep frontline staff up to date on evidence-based best practices to prevent pressure injuries.
We help empower caregivers to fight the 4 contributing factors and keep patients safe with a proven system of products.
Defining the 4 factors that can lead to pressure injuries
When caring for at-risk patients, frontline staff should be considering all the contributing factors of pressure injuries. These important reminders help busy caregivers select the right interventions to keep patients safe.
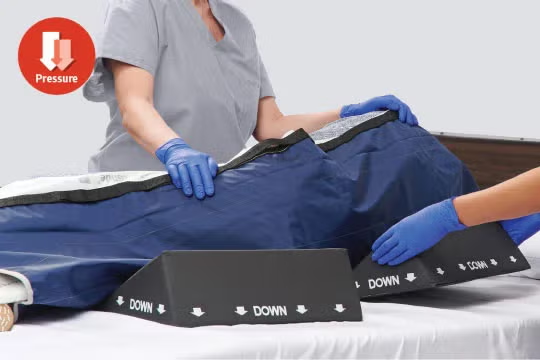
Prolonged pressure
Immobility puts constant force on areas where a pressure injury can develop.
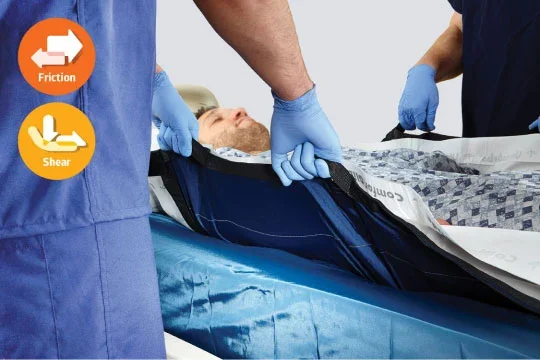
Friction
When skin is pulled across a surface, it injures the outer layer of skin.
Shear
Skin that is pushed in opposite directions can damage deep layers of tissue.
Moisture
Too little moisture or too much can increase the risk of a pressure injury.
Minimize pressure over bony prominences
Pressure on any part of the body can cause skin and tissue damage, but it’s more likely to occur on heels and other bony areas.
Follow NPIAP heel positioning guidelines to relieve the pressure on these bony prominences. A high-density foam wedge and the appropriate supporting surfaces can help lower the risk for pressure injury. Add a prophylactic dressing for heels to increase protection.
Guard against friction and shear
Friction and shear go hand in hand and are particularly damaging for older, thinner skin. Use these strategies as part of your pressure injury prevention protocols:
- The right repositioning system allows you to safely and gently move patients to help redistribute pressure and decrease dragging during transfer.
- A prophylactic dressing helps absorb shear force and reduce friction for pressure injury prevention.1 A transparent hydrogel dressing that reduces peak pressure2 also makes skin checks easier.

Protect the sacrum
A five-layer sacral foam dressing helps manage friction and shear to protect at-risk skin.
Balance moisture more effectively
Excessive moisture or severe dryness can weaken the skin’s natural barrier. That’s why the NPIAP recommends a proven skin care regimen:
- Start with a gentle, pH-balanced foam cleanser.
- Apply a nutrient-rich, dimethicone-based moisturizer to lock in hydration.
- If incontinence is a concern, follow with a breathable barrier cream.
- An absorbant, five-layer foam dressing and moisture-proof dry pads for the mattress can further manage the skin’s microclimate.

Follow a proven skin care regimen
Skin care products with evidence-based ingredients protect and nourish at-risk skin.
Experience our PI prevention products for yourself: Request a sample or demo
Simply complete this form and a Skin Health specialist will contact you soon to coordinate your no-cost sample or demo.

What clinicians are reading about pressure injury prevention
References:
- Sullivan J, Woo K. Comparing the cumulative incidence of pressure ulcers using multi-layer foam dressings in seriously ill patients: a quality improvement project. Surgical Technology International (Reprint) 2018;33:1-5.